Atopic dermatitis (AD
It is a chronic, non-contagious skin condition. Atopic dermatitis almost always begins in childhood. 70 percent of children born into families that have a history of allergic diseases such as asthma or urticaria or hay fever are at an increased risk for developing atopic dermatitis.
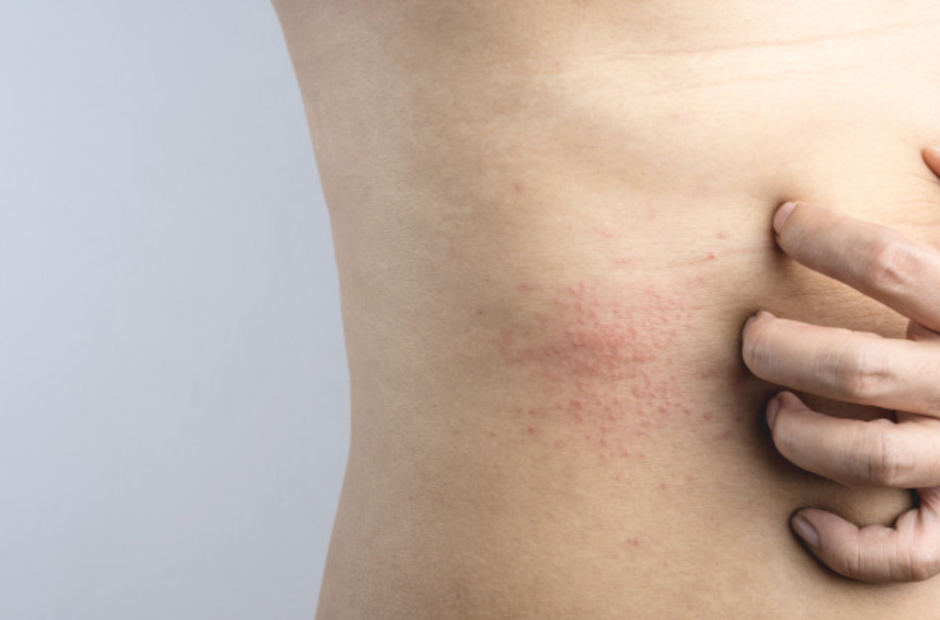
Atopic dermatitis, also called eczema, is a skin disorder that usually appears in babies or very young children and tends to flare periodically. It is a multifactorial skin disease caused by a variety of factors such as genetic conditions. Patients usually have a history of conjunctivitis, allergic rhinitis, cough, sneezing, asthma, especially when weather changes such as in the early morning. Patient family members also have a history of allergy such as allergic conjunctivitis, allergic rhinitis, sneezing, asthma, atopic dermatitis. Food or chemical allergies do not cause atopic dermatitis. It usually happens if skin is overly sensitive to allergens in the environment such as heat, cool, dry, wet, pathogen, and chemical substances irritated skin. People without family atopic dermatitis history may also develop AD because it may be a genetic predisposition without incidence.
The 3 phases of atopic dermatitis
- Infantile stage: It includes children up to 6 – 8 weeks until 2 years of age and is characterized by pruritic, eythematous papules on the cheeks or extensor of surfaces of the extremities and body. The papule may commence after vaccination. The infant with papule shall aware of vaccination or shall consult doctor in advance.
- Childhood stage: The distribution of the lesions changes from the extensor surfaces to the flexor surfaces, particularly the antecubital and popliteal fossae. The skin lesions become more lichenified. As a result of chronic rubbing and scratching, children are easy moody.
- Adolescent/ adult stage: The problem of atopic dermatitis in the infantile and childhood stage may disappear within 2 – 3 years but recur in adolescent stage. The lesions are more severe especially at night. The skin lesions are widely distributed on the antecubital and popliteal fossae, face, shoulder, and upper chest.
Symptom and condition of atopic dermatitis
- Atopic dermatitis is a condition that makes your skin itchy, rash, bumps, blisters, sometimes with oozing and crusting. In chronic case, there is thickened, cracked and scaly skin. The areas of red patches may vary depended on age. In infants at the first year of age, the distribution of the lesions is on the face and head. Some infants may rub their cheeks and head with a pillow, blanket or pad because of itchy.
- In childhood and adult, the distribution of the lesions is on the antecubital and popliteal fossae, neck, face and areas of areas of skin-on-skin rubbing or clothing rubbing against skin. For severe case, the lesions may occur over the body.
- Atopic dermatitis is a chronic skin disorder with intermittent condition. In infants, the skin lesions are usually found around the mouth, on head and neck. In children, the affected areas are located on the antecubital and popliteal fossae, neck, face and areas of skin-on-skin rubbing or clothing rubbing against skin such as elbow, knee. The significant symptom is intense itchy and more lesions when skin is dry, sweating, or bitten by mosquito. The itchy result to scratch and develop an extension of lesion and more infection or complication.
The risk factors for increasing of atopic dermatitis development
- Environment: E.g. pollen, wool, and house-dust mites. These allergens develop more itching.
- Pathogen: E.g. bacteria, fungal. They may cause the skin inflammation or worsen the current inflammation. If you suspect signs or symptoms of inflammation, please consult the attending doctor.
- Season: You may find that AD flare-ups occur more frequently or get worse in the winter. The low humidity, dry and cool air can cause itchy and eczema. Summer months can be dreadful for patients with atopic dermatitis. The summer heat leads to sweat which can irritate the skin, cause itchy and eczema as same as in the winter.
- Clothes: Jewelry accessory and apparel, especially made from wool may irritate your skin.
- Certain soaps, body lotions and detergents: These chemical substances can wear down the oily or/ and contain some components that easily irritate skin and cause itchy as well as dermatitis.
- Food: Food may trigger and worsen 10% of patients suffered from AD. The most common food allergens for children are milk, egg, soy and some kinds of meat.
- Anxiety and stress: These are common triggers that cause eczema to flare up.
Diagnosis
- The diagnosis of atopic dermatitis is based on the findings of the historical features, chronic distribution of skin lesions and chronic with intermittent flares especially at foldable joint areas.
- Allergy skin test such as skin scratch or patch testing or blood test may be used to determine if you are allergic to specific allergens. The common allergens that trigger atopic dermatitis are several.
- Patient and their relatives should observe themselves and avoid all irritants and other things in the environment that can trigger the eczema.
Treatment
- Avoid common triggers to prevent a flare-up of your symptoms such as avoid staying and sleeping in air-conditioned room with very low temperature, avoid shower with cool or hot water, and avoid sweating conditions.
- Take antihistamine to reduce itching. You can treat itching by taking antihistamine two or three times a day วันละ 2-3 ครั้งติดต่อ เว้น 5-7 วัน as needed because itchy may damage your skin and trigger atopic dermatitis. Antihistamine includes chlorphenamine that can buy from general drug stores. Chlorphenamine can make you sleepy.
- Steroid can reduce the inflammation of atopic dermatitis. However, it must be prescribed and used only under close supervision of a caring physician because the long-term use without appropriate advisement may have adverse effect. Avoid a soap that might contain irritating fragrance.
- In case of pustule develops on area of the blisters or widespread red rash, it is a sign of bacterial infection. It is necessary to immediately consult with doctor because it may require antibiotic to kill bacteria.
Tips to hydrate your skin
- Don’t wash in very warm water or wash too frequently.
- Don’t too much washing with soap. Some people misunderstand that itchy cause from unclean skin. The more frequently skin is washed with soap, the more chance of irritation, dry skin and AD flare-ups. Choose a soap that contains skin’s natural pH balance and is free from artificial colors, perfumes or fragrance.
- Add emollients to lukewarm bath water and soak in it or apply emollients straight after a bath. Usually apply a layer of moisturizers or lotions all over your skin for hydrating your skin.
Tips to relieve itchy eczema
- The itch relief can reduce risk of eczema flare up from scratching.
- Avoid clothing that is scratchy, poorly ventilated or tight. Give your clothing an extra rinse, as this will help to further wash out the detergent and softener to stop skin being further irritated.
- Maintain a relatively cool, neutral humidity environment. Avoid extreme temperature changes, too hot or too cold.
- Avoid potential eczema trigger such as perfume, spray, fur, dust, cigarette smoke.
- For people with eczema, sweat from exercise can further dehydrate the skin as well as sting and irritate it. Exercise can also trigger frenzied scratching as the skin surface temperature soars.
- Reduce scratching and always trim your nails short and file your nails round. In children, to prevent those little scratches, it is safe for your baby to wear gloves to bed.
Possible Associated Allergy Diseases
- If the doctor figures out you have food intolerance, try to avoid such particular food allergen.
- If you have other associated allergy diseases such as asthma, allergic rhinitis; you can be treated these diseases at the same time.
- Doctor may prescribe some antipruritics, over-the-counter anti-allergy creams or antibiotics to subside possible associated infections. This problem is a chronic disease that has usually affected your health for years but the particular medication can improve your condition.
- If the atopic dermatitis sufferers strictly follow to physician’s recommendations, more than 50% of them will be released from this problem after the ages of 3 – 5 years. The patents; therefore, should not give up or despond. If you have further inquiry, please consult your doctor.
Common Practice for Atopic Dermatitis
- Don’t too much washing with soap because dry skin is a common finding in patients with atopic dermatitis. Select mild and oil-based formula soaps and apply only in the unclean areas. Try gently rubbing your skin. Don’t soak in the bath for too long. Bath your body by rinsing down with bowl is better than showering. Avoid bathing with too warm water. Dry your body by patting gently with towel and don’t rub or wipe strongly. Avoid clothing that is made from woolen. Wear cotton or well-ventilated clothes. Control your emotion and don’t feel stress. Avoid scratching on the itchy areas.
- Avoid furry pets such as dogs and cats. The allergy-free dogs may be myth, but the understanding about allergy is caused from dog hair is wrong. Allergic reactions from dogs are commonly caused by protein in dander, saliva, and urine. Every dog has such protein. The dog lovers with AD should consult your doctor for an appropriate practice. Avoid taking your dogs into your bedroom. Shower your dog at least once a week. Avoid flooring with carpet because it is difficult for cleansing.
- Avoid kapok stuffing or furry dolls as well as feather pillows. Live in a good air quality environment. Avoid the areas with dusty, industrial chemical, exhaust, spray and gas because they may trigger your AD.
- Be healthy. Cool or respiratory tract infection diseases decrease skin immune and trigger eczema. Away from herpes patients because the herpes virus may transmit to AD patients easily.
- Control your emotion and stress. AD can be triggered by stress. The parents of AD child should not too much worry or be fussy. Don’t scratch because it may damage your skin and lead to bacterial infection.
- The patients and their patients should understand that AD is a troublesome but not life-threatening disease. The patients should accept and learn to live with it. Eventually, atopic dermatitis will get better and will even disappear as they grow.
